Understanding Infantile Jaundice
Jaundice is a word used often in the first week of a baby’s life, but what does it really mean? What causes it, and why are your pediatric providers always so worried about it? Let’s break it down!
Disclaimer: This focuses on what we in the medical community call physiologic jaundice, not breastfeeding jaundice, which is a discussion for a different day!
About 60% of term infants develop visible jaundice in the first week of life. Does it always require treatment? Absolutely not, but it is a top stressor for parents in the first week of life because their babies look yellow and often require frequent trips to the pediatrician. Truly, only about 5-10% of infants develop severe jaundice that requires treatment with something called phototherapy, or blue light therapy.
What is jaundice?
Jaundice is the yellowing of the skin or the eyes in newborn babies. It causes infants to become very sleepy, and thus not eat well leading to other issues, such as dehydration and delayed milk production for mom.
Jaundice tends to peak in term babies (38-42 weeks gestation) between days 3-5 of life, which is after MOST babies have been discharged from the hospital. So, it may seem crazy that your hospital provider (aka me) recommends seeing your primary care pediatrician within 48 hours of leaving the hospital, but this is why.
Why does jaundice happen?
Jaundice is all a part of a baby's body adjusting to life outside the womb.
Babies are born with more red blood cells circulating than adults
Babies need more oxygen carrying capacity in utero than they need after they are born. Their bodies are smart, so their system starts to break down that extra blood supply. The by-product of red blood cell break down in the body is something called bilirubin. When bilirubin accumulates in the blood, it causes symptoms of jaundice.
Babies livers are immature
In utero, the placenta acts partially as the liver for an infant’s body. Meaning, the liver does not receive the signal that it needs to “kick on” to full capactiy until the cord is cut.
The liver’s job in the body is to convert bilirubin into a form the body can remove through the stool (mainly) and urine.
It takes a good 3-5 days for the liver to do it’s job at full capacity, thus why those levels peak between those days and then start to drop.
Babies don’t always eat well in the first week of life
They are sleepy! Especially for the first 24 hours of life. Birth is EXHAUSTING for all parties involved.
Not all babies know how to feed effectively right out of the womb–poor feeding leads to poor stooling and thus, higher bilirubin levels.
The easy breakdown:
Lots of bilirubin production + an immature liver + early feeding transitions = lots of babies with jaundice
Why does it matter and how is it treated?
So, why do pediatricians care so much about these high bilirubin levels in babies? As previously mentioned, in the short term, it can lead to feeding issues and dehydration in infants. Infants do not have the compensatory mechanisms that adults do to deal with dehydration, so it can be very serious for these little ones.
Long term, untreated high jaundice levels can cause something called “kernicterus” which is when plaques form in the brain that cause developmental delays and even death if left untreated.
Most babies never reach levels that would cause this complication, largely because of the safe guards in place to have infants evaluated frequently over their first week of life.
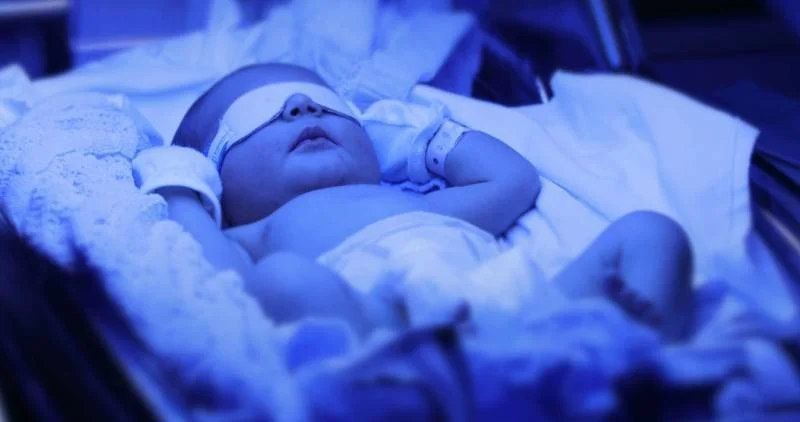
Significant jaundice is treated with something called blue light therapy, or phototherapy which helps the body to break down the bilirubin and eventually stool it out.
Have you heard of infantile jaundice? Did your baby experience it? Did it cause you to stay in the hospital longer than expected?
Check out my Instagram @nuanced_newborns for more information on infantile jaundice and for tips and tricks to survive early parenthood without feeling like you are living at your pediatrician’s office.